Nicola Prentis (@NicolaPrentis / 13/09/17 article) is a mum of two little boys, and she has kindly agreed to share her story of maternal request refusal here to highlight the resistance to caesarean choice that still exists 6 years after NICE CG132 recommended support for all women:
“This was the experience I had in 2015 with my first baby under Bart’s Health NHS Trust at The Royal London. Although I did make an official complaint to the Trust (which they replied to, promising to review the ‘pathway’, and saying they had spoken to the consultant I focused my complaint on), I can imagine that other women might still receive the same attitude from the doctors and hospital there [Note: Nicola is correct – see example below].
At my 10 week pregnancy confirmation appointment, I told the (locum) doctor I would want a c-section. He had no skin in the game since he was only there temporarily, but he warned me I’d have to fight for it. At a later appointment with the regular GP/ obstetrician at Albion Health Centre, I said the same thing and asked how the referral process worked. Her manner instantly became frosty and she replied, “I’ll refer you to the consultant and he’ll say no.” I was a bit taken aback at the bluntness, and how easily she felt she could tell me what I wanted didn’t matter. I asked how that was ‘elective’ and what about ‘patient choice’ and she said the choice was down to the consultant, not me. That began the anxiety that was to last until 37 weeks.
I went to my appointment with the consultant midwife who did the standard thing of telling me the risks, asking why, making me sign the form to say I understood etc. and I would say she was fairly neutral compared to the obstetrician (and consultants that I saw later), but it’s not really neutral when someone says nothing about any of the risks associated with vaginal delivery, is it?
Anyway, she said she would refer me to the consultant doctor who would book me in. She even got a calendar out and said what dates the c-section would probably be. I asked if that was it, “Had I got a c-section?” I can’t remember exactly what she said but I definitely left thinking the next appointment with the consultant doctor was almost a formality to book me in for the operation. Nevertheless, I was uneasy, with the GP’s words ringing in my ears; I wasn’t going to be able to fully relax until I had it booked in.
When that appointment came, I waited 1.5 hours before anyone bothered to tell me the consultant wasn’t there that day. Instead I saw a junior doctor for an entirely pointless meeting where again, I had to explain my reasons, and again, she told me about the risks (though only the risks of a C-section, not a vaginal birth). It also became apparent that nothing of what I said was ever being recorded anywhere, as if it didn’t matter.
I rebooked the appointment and the consultant was aloof, uncaring, and robot-like. I explained my reasons again, and showed I had researched statistics and facts, including the percentage of emergency c-sections and interventions at The Royal London (from its own website), and he said what I said was reasonable – but, “I’m not going to do it.”
I argued, and he countered that I might have to have a hysterectomy and, “What if everyone out there [in the waiting room] wanted a c-section?” [Note: This echoes the Dr. McLellan’s ‘floodgates’ defence in the 2015 Montgomery Supreme Court judgment: “if you were to mention to any mother who faces labour that there is a very small risk of the baby dying in labour, then everyone would ask for a caesarean section, and it’s not in the maternal interests for women to have caesarean sections“.]
I said he couldn’t guarantee me avoiding a hysterectomy since he couldn’t guarantee me a problem-free labour. I was in tears by then, asking about my human rights and my rights over my own body. I was 36 weeks pregnant and he said I was welcome to find another hospital. I asked how could I do this with so little time left? When he said the Trust had a policy against this type of request, I said it was just about money but he was unmoving, and I followed him to the reception in a complete state while he made me an appointment for a second opinion.
I had nightmares about that consultant, dreaming I went into labour and then he was the doctor dealing with me – something that could well have happened. In the interim, I called round other London hospitals, with no luck, of course, as it was either too late or they also couldn’t tell me whether the consultant would agree. I was hysterical, at times unable to speak clearly on the phone, and so stressed out. I felt trapped. I wished I wasn’t pregnant. I felt like all the happiness I was supposed to be feeling about having my first baby had been taken away. I was terrified.
Luckily for me, my sister in Gloucester had a much more understanding health practice, and following an email to her consultant, a trip across the country, and an appointment to see him privately, it meant I could be transferred to Gloucester NHS to experience a much more humane approach to a woman wanting some say in her birth choice. Once this was organized, I realised how much anxiety I had been carrying all that time, as it lifted, and I felt excited, like I should have been all along. This kind of stress on a pregnant woman is dangerous and unforgivable, especially when it’s caused by the people who are supposed to be caring about your health.
I went to my second London consultant appointment anyway, at 37 weeks, because I still wanted to be able to go to the hospital 5 minutes away from me, instead of a 3 hour drive across the country. The head obstetrician went through the entire thing with me again, same spiel, but I was much calmer throughout (even when she said the doctors couldn’t be forced to do something they didn’t want to do) because I knew I had Gloucester to go to. She went next door to ask someone else (I don’t know who), then came back and surprised me by saying OK. Next, for the first time in any of my appointments, she put some actual numbers on some of the C-section risks she had mentioned, and they were so low, like 0.01% or something, and I remember thinking “Is that it? That’s what you’ve all been trying to scare me with?” At one of these appointments, I can’t remember which, I was given a leaflet about VBAC which stated all the terrible things that can happen if you have a c-section. It wasn’t even relevant to me as it was my first pregnancy, but nothing balanced about the risks or statistics of either kind of first birth (vaginal or c-section) was ever given or spoken until that last appointment.
She booked me in for the latest date possible (39 + 4 weeks I recall) so that (I felt), if the op was pushed back, I’d be overdue. I think they were hoping I’d just go into labour in the meantime. I didn’t trust them at all, I didn’t feel safe, and I feared the other consultant would be the one doing the operation. So in the end, I went to Gloucester, where I felt like they cared about me as a patient, and I’m glad I did. Gloucester were fantastic.
The way they treated me in London was bullying, They tried to intimidate me into giving up. If they could change their minds at the last minute like that, they could have listened to me from the start, seen that I was making an informed choice, and respected that. I can only imagine they succeed with many patients who can’t go elsewhere or don’t have the emotional or mental resources to keep fighting the doctors.
I’d hate other women to feel as helpless and powerless as I did but, sadly, I hear these stories all the time, so I know it’s all too common.
* * * * *
Looking at this September 2017 review on the hospital’s website, it’s evident that the care of women requesting a caesarean birth is still unacceptable:
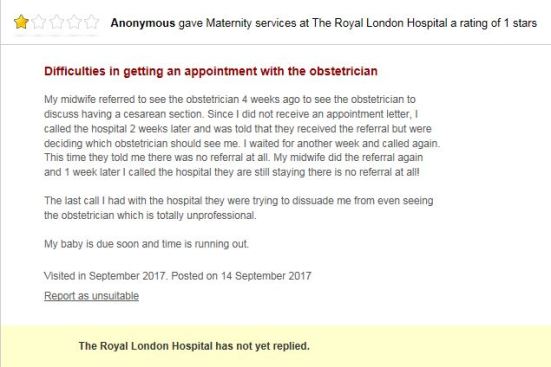
Interestingly, Bart’s Health NHS Trust Maternity page reads:
“We recognise that expectant mothers require very special attention. Our dedicated teams are here to help you through your pregnancy and birth and provide you with the best care to suit your individual needs… From pregnancy through to postnatal care, our team of midwives and medical staff will help you to make informed choices.”
In reality, the menu of choices is limited:
“At Barts Health NHS Trust you can choose to have your baby at one of our tranquil birthing units or in the comfort of your own home cared for by experienced midwives; or in one of our labour wards with doctors close at hand.”
BARTS HEALTH NHS TRUST STATEMENT
Barts Health NHS Trust told Caesarean Birth:
“We are sorry for the distress caused to Ms Prentis and have directly responded to her concerns, having ensured that all our staff are aware how best to advise and support women in their choice.
“Barts Health supports women’s right to choose how and where to give birth, advocating the safest and most appropriate care for women and their baby. The vast majority of women choose to give birth with as little intervention as possible. Women deciding to have an elective caesarean are booked to have the procedure late in their pregnancy, in line with safety guidance by NICE and The Royal College of Obstetricians and Gynaecologists (RCOG).
“We have recently opened a new midwife-led birthing centre, and increased the number of midwives by 40 per cent which is enabling consultants to spend more time with women. We know that there is more we can do to ensure we provide the highest quality care and are currently reviewing the service we provide to all women, as well as improving information leaflets about the risks and benefits of caesareans based on RCOG recommendations.”
I am currently investigating which NICE and RCOG guidance recommends late gestational age caesarean booking, and whether this refers to when a woman’s request would be confirmed too.
Also, a few days ago, I spoke with members of the RCOG’s Women’s Voices team (part of the RCOG’s Women’s Network) about this very issue, and I am hopeful that the College will work together with my organization to ensure that caesarean maternal requests are fully supported in all NHS maternity hospitals.
Women shouldn’t have to be logging on to Mumsnet to ask other mothers which NHS hospitals might be receptive, or where they will need to travel to if their local hospital is not.
- Written and edited by author and journalist Pauline Hull
Thank you so much for sharing this story. I too experienced these same feelings of panic and hopelessness when I thought I was going to be denied. I had been injured by my first vaginal birth and the thought of being forced into that situation (and to potentially endure further damage) against my will was perhaps even more traumatic for me than discovering I had been so badly injured from my first birth. I had been told by the specialist treating me for my injuries that I should give birth to any future babies by csection so was completely blind sided when provider after provider said no. I struggled with waves of intense guilt as I came to the realization that I would rather have not been pregnant with this very wanted baby had I known csection was not an option. During this time I was unable to eat or sleep, my mind was consumed with fear, my blood pressure went up… I even skipped a prenatal appointment not feeling I could face the same dismissive provider again. Thankfully the specialist intervened with a strongly worded letter and I found an OB willinh to help me. Only then did I begin to feel calm and happy about the pregnancy and could focus joyfully on the upcoming arrival. Pregnant woman should never have to experience something like this! I wonder how many more of us are out there…
LikeLike
What an awful and callous way to treat a woman. A woman who had informed herself and made a decision that she felt was right for her and her baby. I thought the first rule of medicine is “do no harm”? It’s quite clear this treatment was damaging to Nicola, particularly in regard to her mental health. I hope the trust and medics involved are ashamed of themselves. I’m not a mom, and when I read experiences like this I question whether I should ever attempt to be one. I too, like Nicola, would want an elective c section. Like it or not we are all different and having thoroughly researched the options and risks I believe it’s the best option for me, my baby, my family, my body and my mental health. We are not just vessels -we are sentient beings, who have the right to informed choice, and who deserve to be listened to.
LikeLike
It is so disheartening to hear what acrobatics women have to go through to give birth by planned cesarean. That choice is perfectly legitimate and a planned cesarean has less risk than a planned vaginal birth. Planning a cesarean or planning a vaginal birth are the only two choices a pregnant woman has.That the ‘experts’ won’t address that issue is a travesty.
LikeLike
Have just finished my masters dissertation regarding PW’s right to refuse c-section but realise it can work in reverse too. “Advocating the safest and most appropriate care for women and their baby…” must entail listening to the women who are actually going through the pregnancy. As set out in Montgomery, the doctor patient relationship is a two way street, not an opportunity for doctors to force their views on patients. Having suffered with anxiety in the past, I fear the limited control that comes with pregnancy, and to think doctors can limit that control even further is enough to make me reconsider having children at all!
LikeLike